Use of HQI’s Hospital Quality Improvement Platform (HQIP) — a quality analytics system that consolidates disparate data sources into a single, statewide platform — continues to increase as more hospitals complete their contract reviews.
The secure, web-based platform, which is free to all California Hospital Association members, provides risk-adjusted quality measures for conditions most affected by hospital quality initiatives. Through the platform, hospitals gain access to clinically rich, timely reports to help easily identify opportunities for improvement and areas for focus. It does not connect to a hospital’s electronic health records system, and uses data hospitals already report to the California Department of Health Care Access and Information (HCAI) and the National Healthcare Safety Network (NHSN). We work for you, so please let us know what reports you would like to see in this platform. The HQI team may be able to create and customize reporting to meet your hospital’s needs.
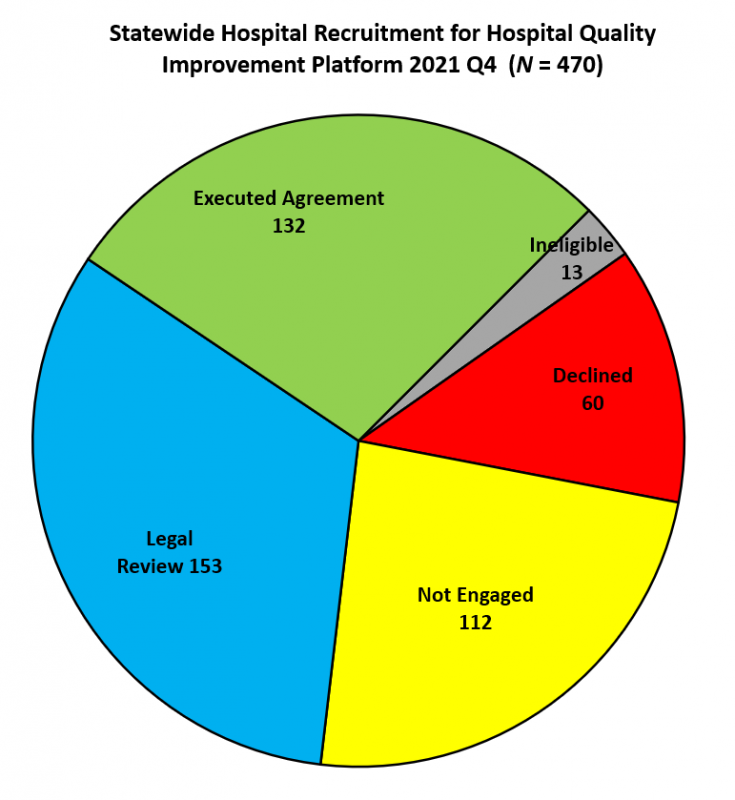
Since launching in October 2019:
- 340 of 470 hospitals have seen a demo of the platform
- 132 hospitals have executed agreements
- 153 hospitals have participation agreements under legal review
WHAT’S IN THE UPDATE
The HQI team is excited to announce that a new-and-improved version of the HQIP will be released in April 2022. The new release features quicker data analytics processing, more flexibility to customize reports, and user-defined multi-level selections for comparison groups and filters, including a slider for choosing the exact time period for your reports. Best of all, HQI staff will be able to add new reports and features to respond faster to customization requests and suggestions. Additional reports and features will be added during each quarter of 2022. We welcome your input about features and measures you would like to see — send them to our HQI technical team at HQIAnalytics@hqinstitute.org.
ABOUT THE PLATFORM
Features include:
- Web-based, completely free, and uses data hospitals already report to HCAI and NHSN.
- Access to hospital performance data from various sources, integrated into a centralized platform.
- Tools to understand your hospital’s quality performance and compare standardized measures to statewide benchmarks and peers.
- The ability to explore same-year quality performance for your hospital, rather than waiting eight to 20 months for statewide files to be released.
- An intuitive interface that provides a window into inpatient and emergency quality indicators.
- Secure data within HIPAA-qualified encrypted data systems.
Quality measures include:
- Inpatient case-mix demographics, comorbidities, index
- Emergency department (ED) discharge analytics (comorbidities, volume, demographics, revisits)
- Ambulatory surgery demographics
- AHRQ patient safety indicators
- Sepsis incidence and mortality
- Maternity measures
- Recent (SIERA) discharge volume by source (inpatient, ED, ambulatory surgery)
- Social determinants of health
- Chronic physical and behavioral conditions
- NHSN measures, trends, and details
There are 15 options for benchmarking your hospital’s performance:
- All CHA member hospitals
- Other critical access hospitals
- Other rural hospitals
- Other children’s hospitals
- Other teaching hospitals
- Your hospital’s past performance
- Other CHA member hospitals:
- In the same health system
- In the same general region
- In the same health service area
- In the same metropolitan statistical area
- With similar bed size
- With the same type of control (e.g., non-profit)
- With the same license type
- With similar Medicare payer mix
- With similar Medi-Cal payer mix
- With the same adult/children’s trauma level designation
- With similar inpatient discharge volume
- With same ED service level (e.g., basic, standby)
- With similar outpatient visit volume
Hospitals can participate by taking three easy steps:
- Execute the cost-free Business Associated Agreement & Master Service Agreement.
- Securely submit copies of recent SIERA/HCAI ED, ambulatory surgery, and inpatient patient-level administrative discharge data files.
- Join HQI’s NHSN group.
For more information about the Hospital Quality Improvement Platform or to schedule a 30-minute demo, visit the HQI website or email HQIAnalytics@HQInstitute.org.